The four most important questions first, in case you are currently considering IVF:
- Will it hurt? Yes.
- Will it be emotionally draining? Yes.
- Will it cost a lot? Yes.
- Will it be totally worth it? Yes, if it works in the end.
Any guarantee? No.
My husband and I wished so much for a baby, a little being to love and impart our knowledge to (and, hopefully, David’s gift of music). David and I had not qualified for adoption, because I wasn’t a US citizen and he was bipolar, so we had to try by ourselves, although I was already 41 by the time we got married in 2014. Curiously, my husband had even kind of predicted our future IVF about 20 years prior in his poem, “In the test tube.” After four unsuccessful IUI’s (Intra-uterine inseminations, where the male’s sperm is injected with a catheter directly through the cervix into the uterus, so it can avoid passing through a possibly hostile vaginal environment), the last one on the fertility drug Clomid, David and I progressed to IVF in 2015, right after our beautiful honeymoon in Hawaii. In-vitro fertilization is when the eggs are harvested from the woman after medical stimulation of the ovaries to produce many follicles, fertilized with the sperm in a petri dish, and then, after a few days of cell growth and division, re-implanted into the uterus as embryos. This way, the embryos can be tested to transfer only the very best and to prevent chromosomal damage. Before you even get there, the woman has to undergo many exams, intra-vaginal ultrasounds (those hurt!) and hormone checks, and be up-to-date on her immunization records, and the man has to undergo a sperm analysis regarding motility and quality. The whole waiting and prepping period took us two years.
Then, we had to wage a war with insurance. After initially promising to cover 85% of the treatment costs, my insurance carrier, CIGNA, had sent me a disapproval letter of the transfer embryo coverage request, after reviewing my case, because in their view, “medical necessity had not been established.” We were really depending on funding. One week before the January 2017 semester started, my employer, Southern Illinois University Carbondale, had laid me off from my part-time French teaching position (SIUC hadn’t gotten a state budget for two years and was laying off lots of non-tenure track faculty). I lost my insurance and was with Health Alliance after that. David was also part time due to his frequent bouts with depression. We had to pay for IVF out of pocket and had already invested the first $5,000. We had taken out a title loan of $10,000 on my bright red Toyota Camry. I had started hormone treatment (Medroxyprogesterone 5 mg, Estradiol 2 mg) to get regular periods and thicker uterine lining, which was checked with repeated intra-vaginal ultrasounds (with the so-called “rape wand”). Luckily, our doctor from Barnes Jewish Hospital, which we had chosen for the procedure, appealed and won the insurance case, so we were finally covered! We “only” spent about $17,000.
Diary entry on the day of embryo transfer:
“YAY!!!! To say it in fertility slang: “Two buns are in the oven!” Of course, it doesn’t mean that both (or either) will implant and develop, but there’s a lot of hope and a good chance.
Last Friday morning, I got the call that from the harvesting on Wednesday, 20 (!!) eggs were retrieved, which is a lot. Out of those, 6 developed abnormally and were discarded, but 14 were incubated for possible transfer and later cryopreservation for another try. I got a call the same afternoon about an update on the fertilized eggs’ development:
1 had 4 cells, 4 had 5 cells, 4 had 7 cells, and 5 had 8 cells.
The ones in the last two categories seemed good for implantation, but the nurse said even the ones with five cells could still make it in the next few days. I was supposed to be on stand-by and wait for a phone call when to come to Barnes Jewish Hospital for the transfer, on Saturday or Monday (today). The embryo transfer is done either on the third or the fifth day after retrieval, depending on the quality of the eggs.
They called Friday evening to say I should come Saturday morning at 8:55 a.m., but that they MIGHT call me on the very day at 7 a.m. when they looked at the eggs under the microscope and postpone to Monday. So we drove off at 6:20 a.m. last Saturday, and we were close to Pinckneyville when my cell phone rang and the clinic called it off to postpone to today!
This morning, I arrived around 8:55 a.m., and then it went very fast. I had to drink a lot of fluid before the procedure, because it’s easier with a full bladder. In the prepping room, I had to take off my clothes, put on an in-the-back-open hospital gown and two blue paper shoes. There was a diary lying on a table, into which prior IVF candidates had written words of encouragement. Most were like, “our 4th trial; good luck; you can do it; thanks to the great staff here; I was successful the 2nd time, trying again,” etc. One was from a waiting male (a sperm donor), and was quite funny: “To the other guys here, if you’d also like better porn, can I get an amen?” -“I didn’t need any porn, just looked at Glamour magazine, haha!” The nurse said I could write in it, too, but there wasn’t a pen, so I didn’t.
The real procedure was less painful than the trial embryo transfer I had undergone the month before (where they sprayed a saline solution into me through the catheter). The worst part is really when they insert the cold metal speculum into your vagina and then use a clamp to fasten the cervix, so they can push the catheter through. Last month, I bled for the rest of the day, because they had hurt my cervix. For the real thing this time, I had taken one of David’s Lorazepam pills for anxiety and two Ibuprofen, and was very brave and calm… whined just three times.
Above, you see the future little Lyons: The first one is Emily Rosalyn, and the second Leander David 🙂 (Of course we can’t tell the gender yet. David had hoped they would implant the gender you wished for, because he wanted a daughter – they do that somewhere in the country, but Barnes Jewish Hospital doesn’t screen for gender.) I want a boy, so if we have twins, there might be one of each. Nice round and sharp morulas, don’t you think?
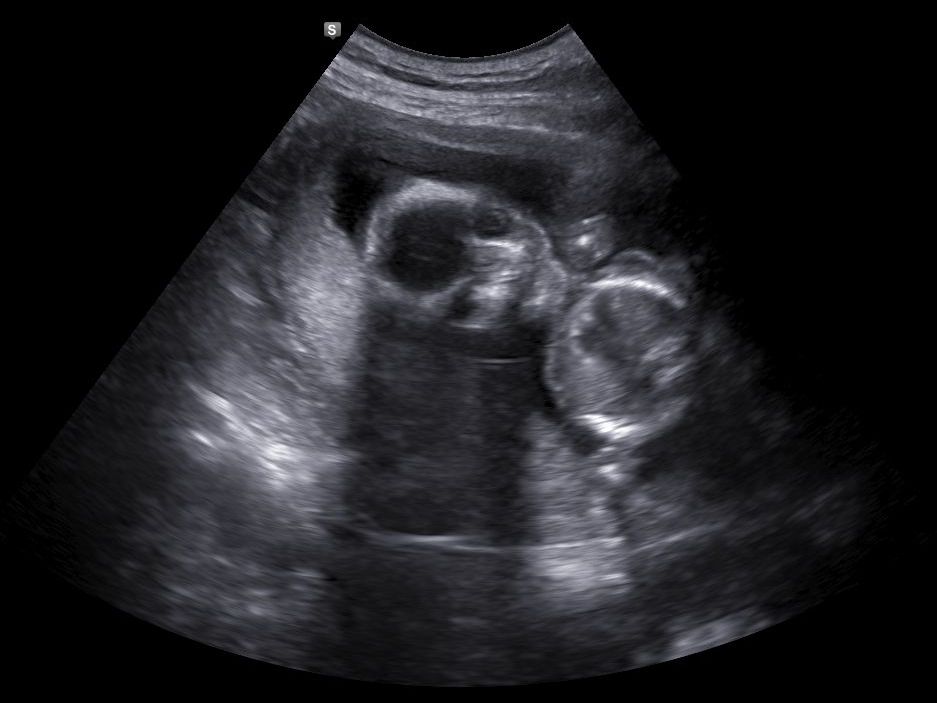
They let me watch the transfer on the ultrasound monitor. What you’re supposed to see in the ultrasound below is a nice, healthy, slimy uterus with a very full bladder on top, and the long needle coming from the right side and depositing a shiny, white air bubble with the two embryos into it! What I saw was a unicorn:

I described it to the nurse, and finally, she saw it, too, and said I could make that the theme ofthe nursery 😉 In a few days, I’ll get a call from the clinic to hear how many out of the 12 remaining embryos were worthy for cryopreservation. If it doesn’t work this time, I can do an IVF cycle with my frozen embryos next time, after a month’s rest. Frozen cycles are much cheaper, since I wouldn’t have to pay for the stimulating medicines and surgery anymore, and in the past, they had a 2/3 chance of developing into a pregnancy when compared to fresh cycles, but in the recent years, the clinic says there is hardly a difference anymore between fresh and frozen cycles.
Right after the procedure, I had to lie still for about 30 minutes, and then I could be driven home again. And no, the embryo couldn’t fall out of my body, not when walking, not when coughing, not when sneezing, and not when peeing. I don’t know where this irrational fear comes from that makes women tread like on eggs after the transfer. I had googled that already, but I was still really, really worried the “embies might not stick” or move around in there, or attach to the wrong spot. I had spent countless hours on fertility forums such as “The Bump” and picked up their slang: Baby dust to all!”
The worst thing after transfer day is the feared “2ww” – the two weeks’ wait. In the meantime, those nasty progesterone shots with a long needle in the butt, the prenatal vitamins, and estrogen pills continued. I wasn’t supposed to lift anything heavy (not easy when you’re about to move states for a new job). After two weeks, you can “POS” (= pee on the stick) to see if pregnancy hormones are detected in your urine, and you get your blood test (the first beta) at the Obgyn’s office. Many women can’t wait that long and succumb to POS before the right time, and then they freak out about a negative pregnancy test, or they see an imaginary line and ask other forum members if they could see it, too… I read the forums like crazy, but I abstained from POS too soon. Instead, I did what the other forum ladies did: I charted each and every symptom, hoping it was a pregnancy symptom and not just a bloat from eating too much, and compared mine with the other ladies’ symptoms. My tip: don’t do that. Drives you nuts.
- day of IVF: mild cramps, cervix hurts, slight nausea
- day 1 post transfer: mild cramps, slight nausea
- day 2 post transfer: tired and runny nose
- day 3 post transfer: runny nose and bloated, constipation
- day 4 post transfer: sex dream w/orgasm at 5 a.m., runny nose, constipation
- day 5 post transfer: insomnia, slight cramps, runny nose, constipation
- day 6 post transfer: brownish slimy discharge, runny nose, insomnia, sore nipples
- day 7 post transfer: slept until 10 a.m., runny nose, sore nipples, belly more bloated
- day 8 post transfer: insomnia, belly much bigger, veins on right boob, sore throat, still stuffy nose, sore nipples
- day 9 post transfer: stuffy nose, break-out on chin, asthma
- day 10 post transfer: stuffy nose, break-out on chin, asthma
- day 11 post transfer: stuffy nose, break-out on chin, New Horizon Obgyn 8 a.m. blood test!!!! first beta 541
- day 19: second beta: 5,642, doubling rate: 2 days 9 hrs (=57 hrs) normal
- day 32: I am 7 weeks 1 day pregnant (first ultrasound!), 9 mm, heart beat 138
I faithfully continued this diary until Day 231 post transfer, or 34 weeks and 6 days pregnant, when baby was born. How sad and disappointing that at my first ultrasound at 7 weeks at the Obgyn’s office, there was only ONE little gummy bear, and not two! I learned that I had had a “vanishing twin.” He or she had gotten absorbed by me or the remaining twin. But there was still one little beating heart to fight for! At seven weeks pregnant, I had to go to the hospital for a severe asthma attack brought on by cleaning out David’s guinea pigs’ cage and handling dusty moving boxes. I was afraid to loose my only one then, but all was fine. The next day, I moved to Clarksville, TN. Although I was regularly supervised by my Obgyn, I still went to an elective ultrasound at LoveMyBabyBump every three to four weeks, just to make sure the little one was still there and thriving. I needed that peace of mind after the sudden loss of my husband.
At 12 weeks pregnant, I did a gender ultrasound, but it was really too early to see much. I was told I most likely expected a girl, and I would get a confirmation at my 15-weeks gender scan, when it could be seen for sure. So I already started to buy pink clothes for Emily Rosalyn. However, at my 15-weeks scan, it became clear that Leander David had just tucked away his private parts really well before:
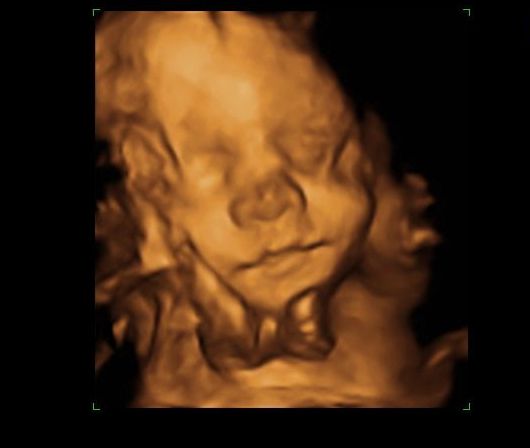
Two weeks later, one could see the face clearly already. However, I wondered if I was having an alien:
I was diagnosed with partial placenta previa during my ObGyn ultrasound appointment in week 20, which means my placenta was covering up the cervix, which can lead to heavy bleeds in the third trimester and *might* require a month of bed rest; in the worst case, in the hospital. It can also cause preterm labor. I would be classified high risk then. If that were to happen, I wouldn’t be able to travel or work at all. However, the doctor said since my uterus was still growing, there was a chance that the placenta moves upwards. If not, they would have to get the baby through C-section, because his exit way was blocked. They would let me know in mid-November at the next appointment whether it had moved or not. According to the Internet, in 80% of women with partial placenta previa, it moves higher in the third trimester, and all is fine.
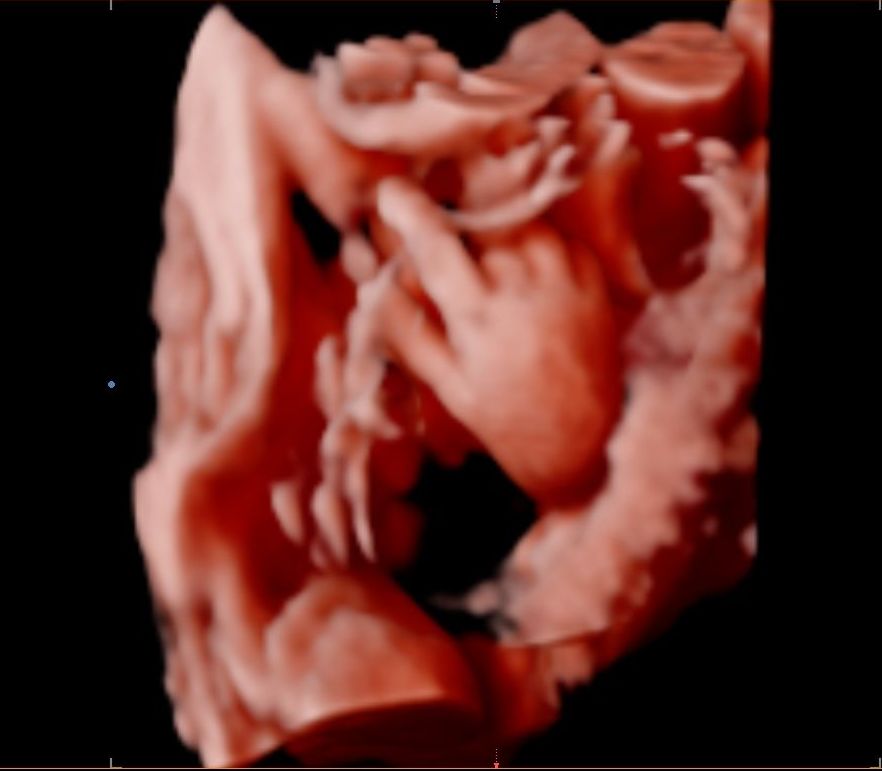
At 21 weeks, Leander David was surprising me by his gestures on the ultrasound. Doesn’t it look like he’s catching a baseball on one of the pictures? Maybe that’s an omen (although I really wanted a piano player)… On the other picture, it looks as if he were saying, “Oh no, she is looking at me again…” By the way, there are some conspiracy theories to the effect that frequent 3D ultrasounds could be bad for baby, or even cause autism. There is no scientific research to back that up. If it’s not medically necessary, one should avoid them, but when you do IVF, you will most likely receive more ultrasounds than other mothers, anyway, especially when you are high risk or end up with problems like placenta previa. When I gave birth, they feared placental abruption, which luckily did not happen. It can be dangerous to mom and baby, and you can lose a lot of blood.
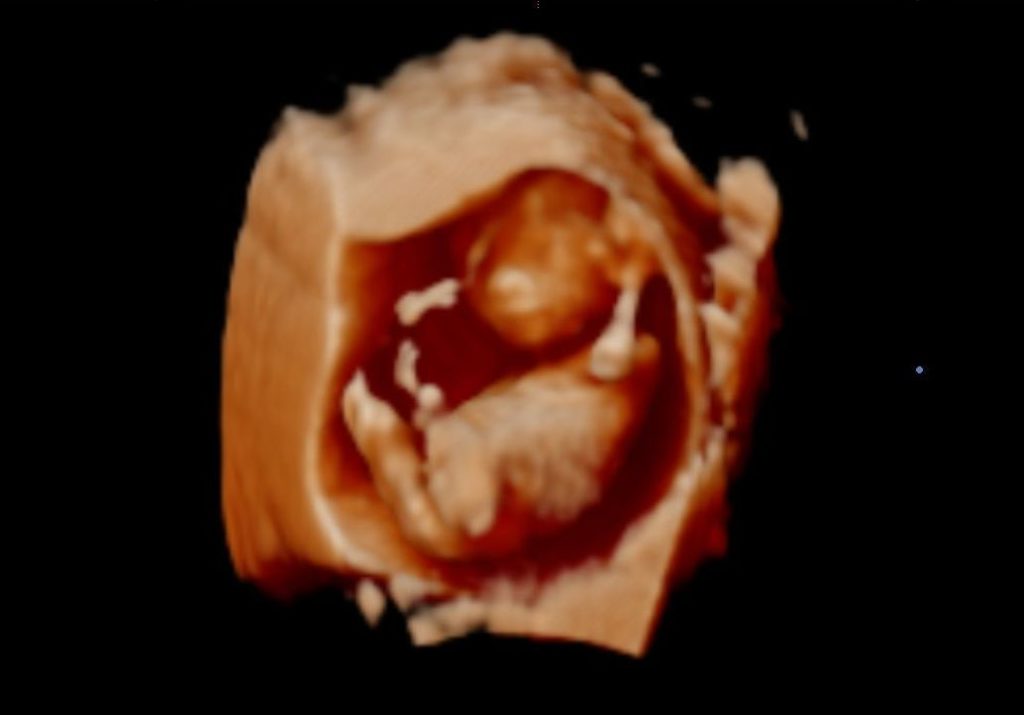
At 24 weeks, when my baby reached viability, I was able to relax a bit more. He measured on track, just a little bit on the smaller side, so if he had to be born early, there was a good chance that he’d survive. I had been a 7-months child myself, so I anticipated that he would arrive somewhat early. My favorite 3D ultrasound was taken in Michigan, when I visited my late husband’s brothers at 25+2 weeks pregnant. We went to a studio to watch a 20-min. movie of what was going on in my belly, and they took a few still images for us. On one of them, it looks like Leander David was wearing a bow tie! He got all dressed up to meed Daddy’s family.
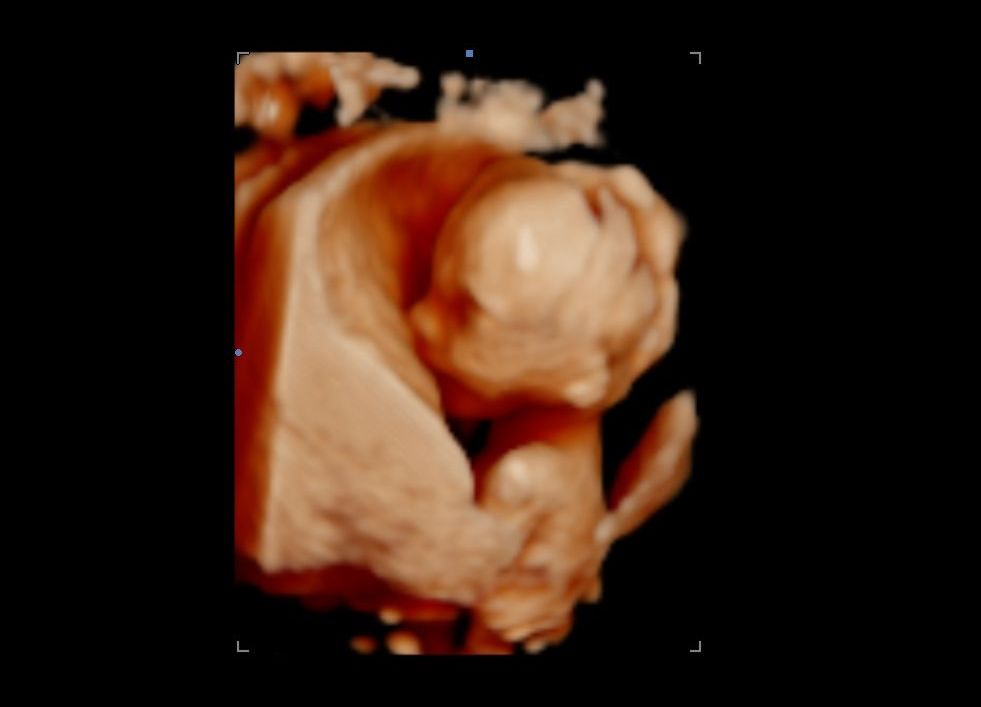
The good thing was that my partial placenta previa had resolved. I had my last Obgyn appointment at 27+2 weeks; otherwise, they would have noticed that my son stopped growing around 28 weeks due to a malfunctioning and tiny placenta. At 31 weeks at the elective ultrasound, he filled out the ultrasound so much already that one could only see a hand, a foot, and an ear.
I had passed the first glucose test (yuck; they make you drink a whole little bottle of terribly sweet sugar water, and then you have to sit in the waiting room for an hour, until they take your blood. It was so disgusting; I felt a little sick afterwards). However, I failed the second one and had to repeat it, but the results (which were okay) were not in before Leander was born. He arrived at 34 weeks and 6 days, weighing 3 lbs (he had IUGR) and requiring three weeks of NICU. On my dismissal papers it read, “geriatric, diabetic mother.” In spite of this, my pregnancy had been a very pleasant one, without nausea and other troubles except for pregnancy rash that came and went. It was almost gone by the time I gave birth. The 12 weeks of progesterone injections in the beginning were not pleasant, but it’s a small sacrifice to ask. Just make sure you give yourself the shots in your butt, not in your leg, because I did that once and hit a nerve, and needed to lift my leg into the car, because it wouldn’t move by itself for a day. There were lots of YouTube videos to explain how to administer the shots if you don’t have a husband who could do it for you (or if he is scared to, ha!). I also binge watched, “I Didn’t Know I Was Pregnant,” and visited online forums for support. IVF was a great experience and definitely worth it. For me, it worked the very first time ’round, and to you out there who are still trying, I wish great luck!
And for those who got pregnant: Congratulations!! Now might be a good time to set up a Baby Registry from Amazon. You’ll be busy with medications and taking care of yourself, and you’re still reeling from the costs of IVF. Your friends and relatives might want to send you something to show their support. I set up a baby registry for my son and received many useful items, such as clothes, bottles, crib sheets, toys, etc. It will prevent you from receiving things that you already have, or that another person wants to send you. It is especially valuable during the pandemic, because many relatives cannot visit you, but they really want to contribute in some way. Also, you won’t need to go physically shopping with mood swings due to the IVF medications or hurting from the progesterone needles (I put one progesterone shot into my leg instead of my butt once, and had to lift it into my car to drive, because I had hit a nerve!), since the items are delivered directly to your door to any address you indicate. For me, it was a big help during a difficult time. (Disclosure: This is an affiliate link. This means that, at zero cost to you, I will earn an affiliate commission if you click through the link and finalize a purchase. It’s a win-win, because this way, you can help a little half-orphaned boy a bit, too. My husband sadly and unexpectedly passed away in 2017, months before our son was born (it was a difficult birth; our boy had IUGR, came at 8 months, and weighed only 3 lbs).)













So beautiful, all of it, the honesty and details. Thank you.